Yes. Stress can trigger IBS flare-ups, and for many people it does so more consistently than any food. The gut and the brain are physically connected through nerves, hormones and the autonomic nervous system. That connection runs both ways, which means what happens in the mind shows up in the gut, often within hours. Bloating, urgency, cramping and irregular bowel habits can all intensify during stressful periods even when the diet stays exactly the same. At Total Health Center in Virginia Beach, this connection is part of every digestive evaluation from the start.
How Stress Actually Affects Your Gut
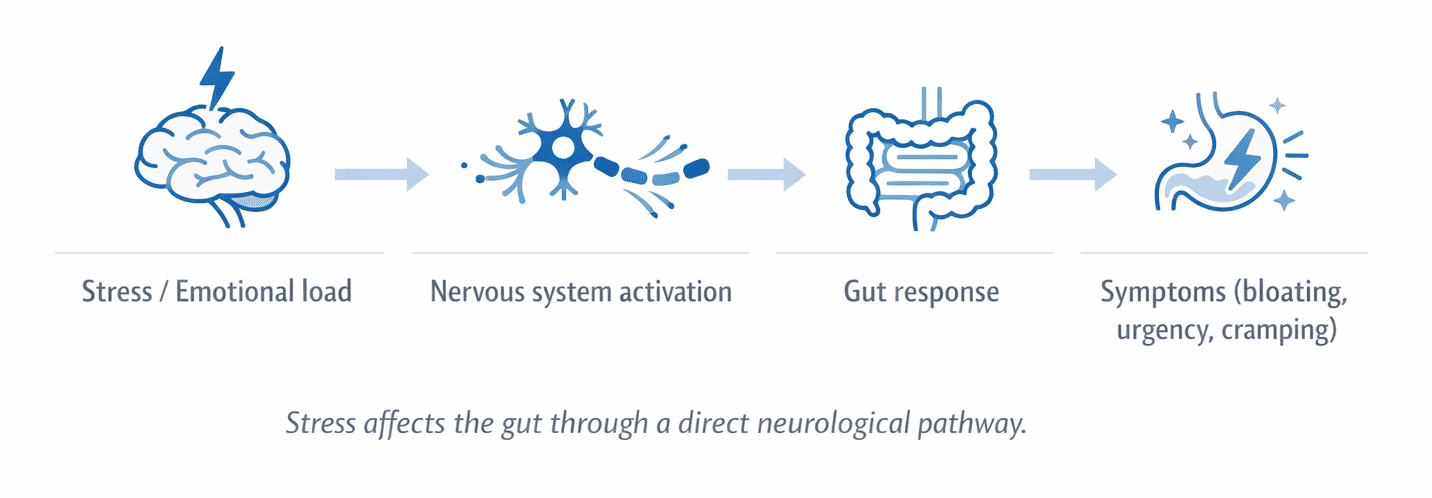
The digestive system has its own extensive network of nerves, in direct communication with the brain through hormones and the autonomic nervous system. When stress activates the body’s threat response, that communication changes fast and the gut feels it immediately: digestion speeds up or slows depending on the person, muscle contractions shift rhythm and sensitivity to pain increases. For someone without IBS these changes may be barely noticeable. For someone with IBS, whose gut is already running at a higher baseline of reactivity, the same stress response can tip into a full flare.
The brain and gut are physically connected. Stress has a measurable, documented effect on how the digestive system functions.
What It Actually Looks Like Day to Day
Most people recognize this pattern the moment they see it described. Symptoms that do not follow a meal but consistently follow a situation: a deadline, a difficult conversation, a week of broken sleep.
Common stress-related IBS patterns that come up repeatedly at Total Health Center:
- Urgency or cramping on Sunday nights before a difficult work week
- Loose stools during periods of sustained pressure at work or at home
- Bloating that builds during demanding stretches and eases on vacation
- Cramping that has no clear food connection but tracks closely with sleep quality
- Symptoms that improve on weekends and return Monday morning
If your gut seems to have a calendar, that is useful clinical information. It points toward a nervous system component worth factoring into a complete evaluation. Dr. Scott looks at this pattern from the first visit at Total Health Center, because stress timing often explains what months of food tracking left open.
Why Food and Stress Are Hard to Separate
Many patients arrive having tracked their food carefully for weeks without surfacing a clear trigger. What the evaluation often reveals is that stress level is the variable driving the pattern. The same meal lands fine on a calm day and causes a real flare when the week is heavy, the sleep is poor or the emotional load is high. The gut responds to the body’s full state in real time, and when any of those variables shifts, gut sensitivity shifts with it.
Portion size, sleep quality and emotional load all interact with what was eaten, which is why the functional medicine approach at Total Health Center looks at all of them together. Patients dealing with both food and stress triggers get a clearer picture when both are evaluated at once. More detail on how food fits into this is at Digestive and Metabolic Health.
When to Stop Managing This on Your Own
Most people with stress-related IBS have already tried the obvious adjustments: cutting caffeine, avoiding trigger foods, bringing stress down where possible. Sometimes that helps meaningfully. A complete evaluation tends to move things further, because it looks at the gut-brain component directly alongside everything else.
A complete evaluation changes the picture. At Total Health Center, the first visit includes a review of health history, symptom timing and lifestyle patterns, and when it makes sense, targeted lab work to understand what is actually driving the flare-ups. Patients who have been managing IBS symptoms on their own for years often find that the first evaluation surfaces a connection they had been looking for.
The Total Health Center approach is built around root cause. When stress and digestion are tangled together, that starting point makes all the difference.
Get Personalized IBS Support in Virginia Beach
If your IBS symptoms track closely with stress, sleep or emotional load, a proper evaluation gives that pattern the attention it deserves. Total Health Center offers a focused first visit built around your specific history and symptom picture. Call (757) 363-8571 to schedule.
Frequently asked questions
Can stress actually cause IBS?
Stress activates a direct physiological response in the digestive system. In people with IBS, that response is amplified and can trigger flare-ups on its own.
Why do my symptoms improve on vacation and come back when I return?
That pattern is a clear nervous system signal. The gut is responding to a lower stress load. It is one of the most useful pieces of information in an evaluation.
Can I have both food and stress triggers?
Yes, and it is common. Most patients with stress-related IBS also have some food sensitivity. Both need to be addressed for consistent improvement.
Will managing stress fix my IBS?
For some people, yes. For others, stress is one factor among several. An evaluation helps determine how much weight it carries in your specific case.
