Contact Us
Tel: (757) 363-8571
Digestive symptoms often have more than one driver. In functional medicine, the goal is to identify patterns across digestion, immune signaling, inflammation, stress response, and nutrient status, then use targeted testing only when it adds real clarity.
At Total Health Center in Virginia Beach, digestive concerns are evaluated through a comprehensive lens that considers how different body systems interact. Dr. Mark A. Scott has worked with chronic digestive cases for over 28 years, many involving patients who’ve tried standard approaches without lasting relief. The focus is on understanding what’s driving symptoms so care can address those factors directly.
What a Functional Medicine Digestive Evaluation Focuses On
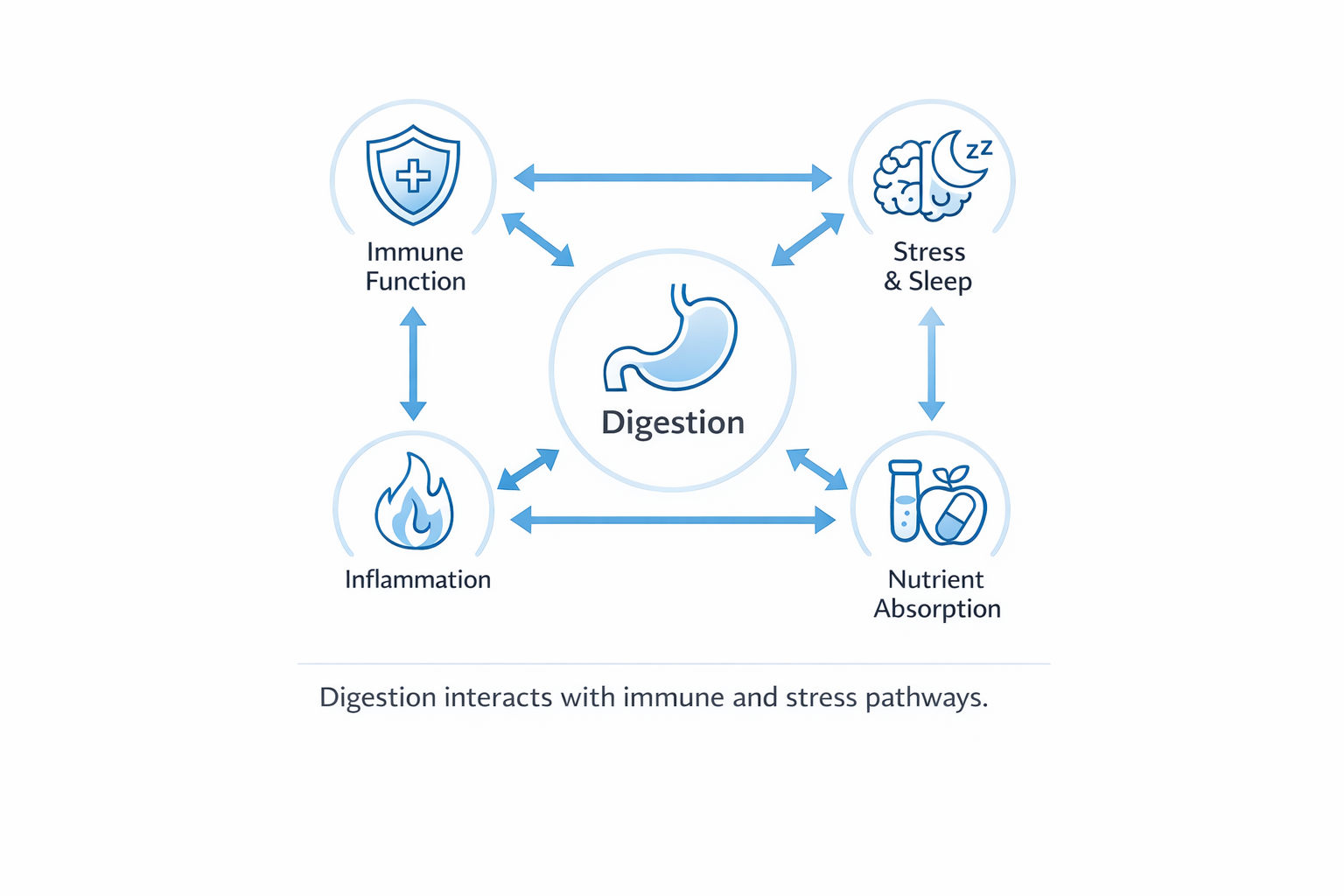
Digestive function influences nutrient absorption, immune regulation, and inflammatory signaling, so symptoms can show up beyond the gut (fatigue, skin changes, joint discomfort).
A functional medicine digestive evaluation typically looks at:
- Symptom patterns (timing, triggers, and what improves them)
- Stress + sleep impacts on mobility and gut-brain signaling
- Medication and supplement history (what may be shifting the microbiome)
- Possible post-infection or immune shifts
- Nutrient absorption patterns that affect energy and inflammation
The goal is a clearer map of what may be interfering with normal digestive regulation, and what deserves attention first.
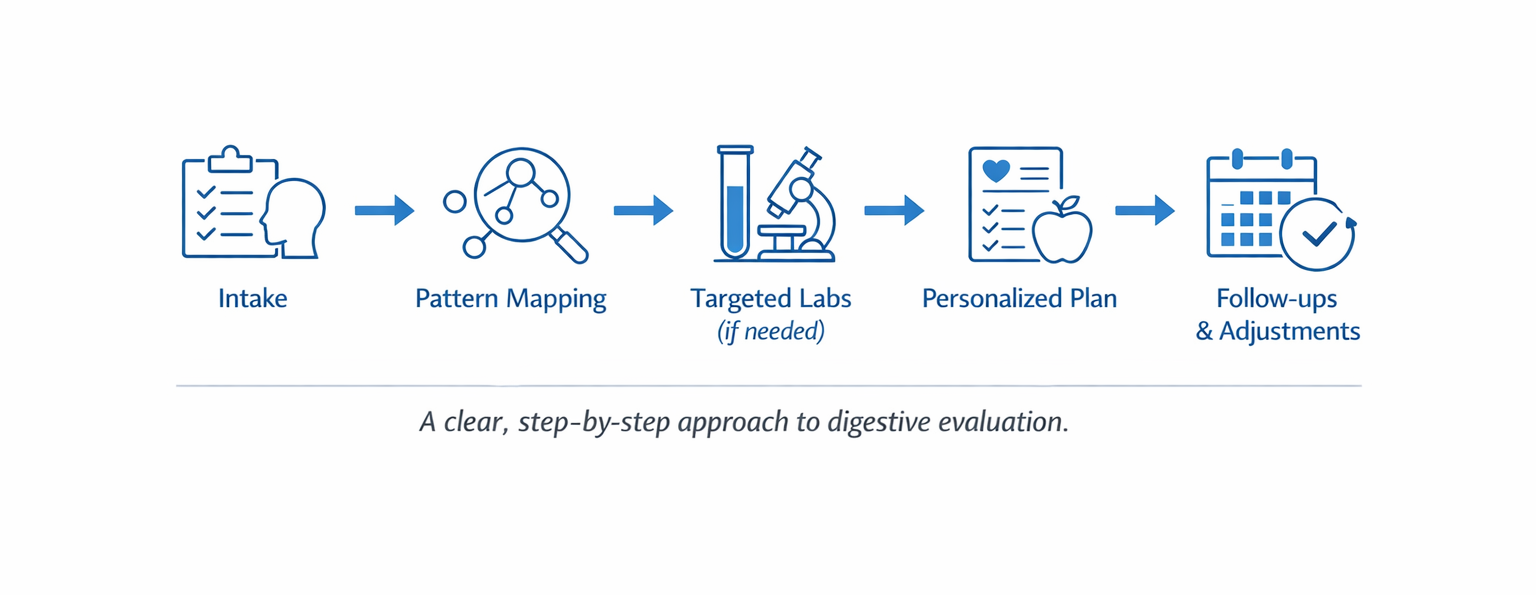
Clinical Intake: History, Triggers, and Overlapping Factors
The evaluation starts with a detailed health history. Dr. Scott reviews when symptoms began, what’s been tried before, current medications, stress levels, sleep quality, and dietary habits. Each element provides context that typical consultations may not capture in depth.
Digestive symptoms rarely exist in isolation. Stress alters gut motility, medications can disrupt microbial balance, and past infections may trigger longer-term immune changes. Many patients arrive after trying multiple approaches without lasting clarity. Mapping how these factors overlap helps explain why symptoms persist.
The goal is to map out a complete picture so recommendations can be targeted and precise.
Targeted Lab Testing (Only When It Adds Clarity)
Testing is used selectively based on what the clinical evaluation suggests. At Total Health Center, lab work is chosen according to the individual case, focusing on what will provide useful clarity.
Common areas of assessment:
- Digestive enzyme activity
- Gut microbiome composition
- Inflammatory markers
- Intestinal permeability
- Nutrient absorption patterns
Results are interpreted within context. A finding that looks normal in isolation may be clinically significant when viewed alongside other patterns. The purpose is to clarify what clinical evaluation alone cannot determine and to guide more precise interventions.
This differs from standard testing in that it looks for functional imbalances where the body is compensating but struggling before clear pathology develops.
When Functional Medicine Is Most Helpful for Digestive Symptoms
Functional medicine for digestive health is especially relevant when symptoms persist despite effort or when previous evaluations have provided incomplete answers.
Common presentations include:
- Bloating, discomfort, or irregular bowel habits that continue despite dietary changes
- IBS-type patterns without clear resolution
- Symptoms that improve temporarily but return
- Interest in understanding root contributors and addressing them directly
This approach complements medical care. It’s designed to support better long-term digestive function, particularly when standard treatment has reached its limits.
How Digestive Care Is Integrated at Total Health Center
At Total Health Center, digestive care is approached as part of an ongoing process rather than a one-time intervention. Insights from digestive evaluation are used to understand how gut function may be influencing other areas such as inflammation, metabolism, immune response, or weight regulation.
For some patients, digestive symptoms are the main reason they seek care. For others, digestive imbalances emerge as contributing factors while addressing broader concerns. In both cases, digestive findings help guide priorities and shape how care evolves over time.
As patterns shift and the body responds, recommendations are adjusted accordingly. The focus remains on helping patients understand what is happening, why it matters, and how each step fits into their overall care.
Integration of Functional Medicine With Other Care Modalities
Functional medicine care provides the diagnostic and strategic framework. Nutritional counseling translates findings into actionable dietary and supplement recommendations. Chiropractic care addresses structural and nervous system contributions to digestive regulation.
This integrated approach reflects reality: digestive function is influenced by stress response, spinal alignment, nutrient status, and inflammatory signaling. Addressing these in combination often produces better outcomes.
What to Expect During an Initial Functional Medicine Visit
The first visit includes a thorough review of health history, a physical assessment, and a discussion of symptoms in context. Dr. Scott explains the functional medicine perspective, what testing may be appropriate, and what the process typically involves.
Patients are encouraged to ask questions and share their observations. Understanding what’s happening internally helps patients make informed decisions and follow recommendations more effectively. Follow-up visits track progress, adjust protocols as needed, and address any new patterns that emerge.
Schedule a Functional Medicine Evaluation for Digestive Health
Total Health Center offers functional medicine evaluations for individuals dealing with persistent digestive concerns. The initial visit includes a detailed health history review, physical assessment, and discussion of testing options based on your specific case.
Appointments can be scheduled by calling the office or booking online. Dr. Scott and the team work with patients to identify contributing factors, develop personalized protocols, and support long-term digestive health through education and ongoing care.
