Most people with IBS get good at reading their own body. They know what a bad week looks like, which foods tend to cause problems and roughly how long a flare lasts. That familiarity is useful, because it makes it easier to notice when something sits outside the usual picture. When symptoms change character, show up in new ways or stop following the familiar IBS rhythm, that shift is worth taking to a clinician. At Total Health Center in Virginia Beach, Dr. Mark Scott looks at these patterns when a patient’s digestive history has more pieces than a standard IBS diagnosis captures.
How to Tell When the Pattern Has Shifted
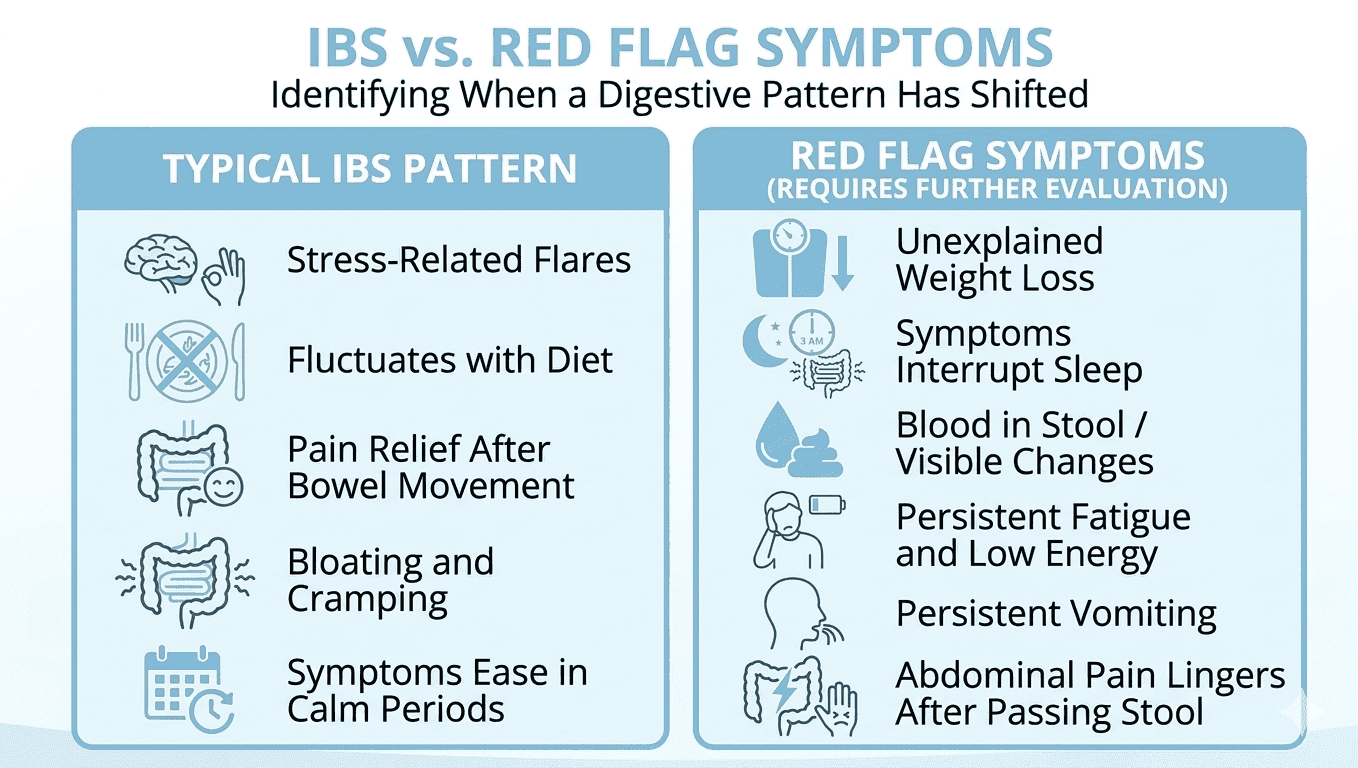
IBS has a rhythm. Symptoms fluctuate with food, stress, sleep and routine. On a difficult week they get worse, on a calmer one they ease. The symptoms below behave differently. They tend to persist regardless of diet or stress changes, and several of them reflect processes that fall outside what IBS typically produces.
Changes in stool appearance that go beyond your usual IBS pattern. Stools that are consistently dark, tarry or show any sign of blood are worth bringing to a clinician. IBS affects consistency and frequency, but visible changes of this kind point toward something else the digestive tract is doing.
Losing weight without trying or without a change in diet. IBS can make eating uncomfortable and disrupt appetite, but consistent weight loss without an obvious reason points toward a process worth investigating. It is one of the clearer signals that something beyond a motility issue may be at play.
Fatigue and low energy that does not lift. Iron-deficiency anemia can develop quietly alongside digestive symptoms. When fatigue is persistent and unexplained, checking iron levels is a reasonable step.
Waking up at night with digestive symptoms. IBS responds to the nervous system and digestive rhythm during waking hours. Symptoms that interrupt sleep are following a different physiological path, and that distinction matters clinically.
Vomiting that keeps coming back without a clear cause. Occasional nausea tied to a difficult IBS day is one thing. Persistent vomiting unconnected to illness or a specific food reaction is worth evaluating.
Abdominal pain that stays after a bowel movement. IBS discomfort typically eases once the bowel empties or gas passes. Pain that lingers afterward is worth flagging with a clinician.
Each of these signals that the symptom picture has expanded enough to warrant a proper conversation.
Why These Symptoms Are Easy to Dismiss
People who have lived with IBS for years tend to absorb new symptoms into the existing diagnosis. Something feels off, but the assumption is that it is still the IBS. That instinct is understandable, and it is also the reason a more complete evaluation often surfaces things that had been part of the picture for longer than expected.
Unexplained weight loss is a good example. IBS can make eating uncomfortable and disruptive, but weight dropping consistently without a clear dietary reason points toward a process the gut is managing on its own. Iron-deficiency anemia without an obvious source often signals that blood is being lost somewhere in the digestive tract, even when nothing is visible externally. These are subtle distinctions from the outside. They are exactly what an experienced clinician is trained to read.
At Total Health Center, Dr. Scott has worked with patients whose symptoms had been attributed entirely to IBS for years before a more complete evaluation revealed what was actually driving the picture.
When the Right Move Is a Full Evaluation
A pattern that shifts in character, intensifies consistently or produces new symptoms is telling a different story than typical IBS fluctuation. These are the situations where a proper clinical evaluation makes sense:
- A symptom that is new and has no clear connection to food, stress or routine
- The familiar IBS pattern has shifted in a way that feels qualitatively different
- Digestive symptoms are affecting sleep, work or daily function more than before
- Any of the warning signs described above are present, even occasionally
- Months of dietary and lifestyle changes have produced limited results
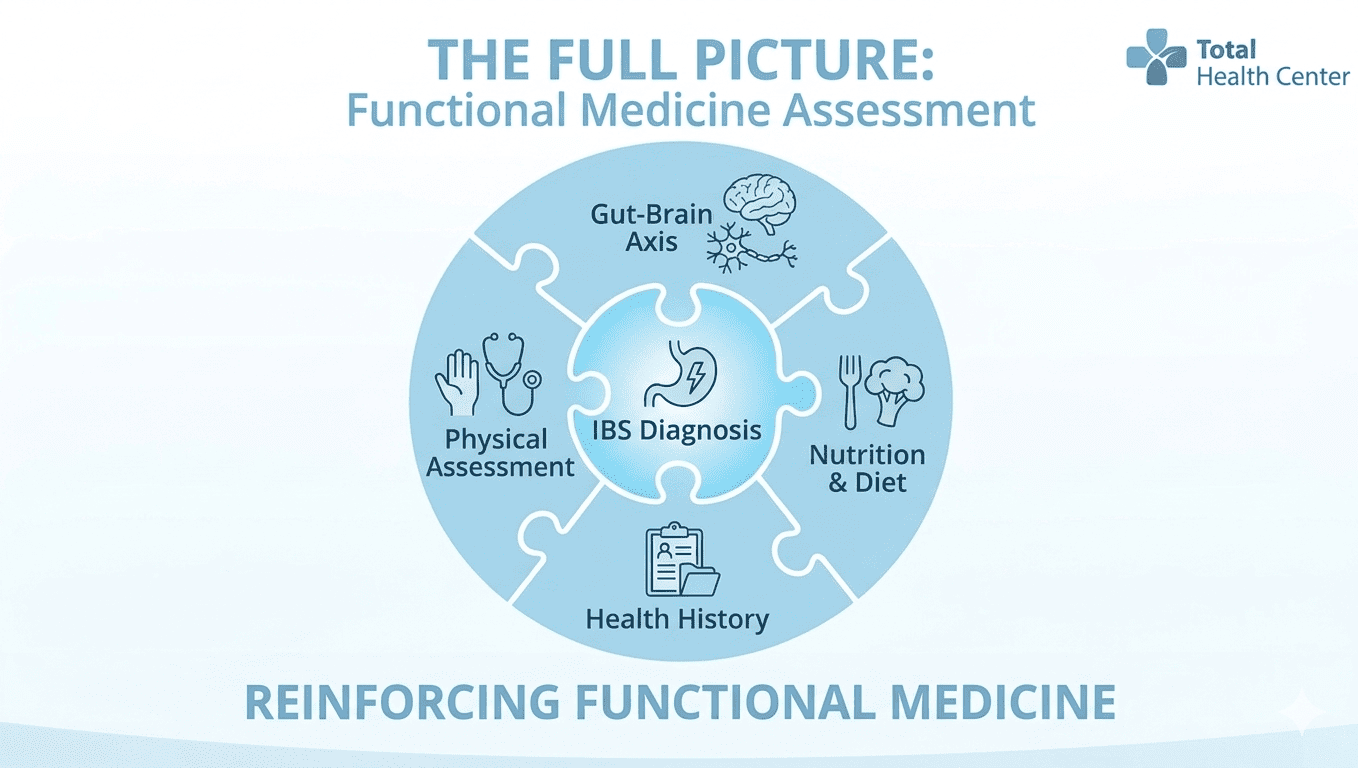
At Total Health Center, the first visit covers a focused review of health history, a physical assessment and a direct conversation about whether lab work is the right next step. The functional medicine approach starts with understanding the full picture, which is how patterns that have stayed unresolved for years often become clearer.
Conditions That Share Symptoms With IBS
Several digestive conditions produce symptoms close enough to IBS that they are worth evaluating alongside it. Celiac disease frequently causes bloating, abdominal pain and diarrhea in patterns that overlap significantly with IBS. Crohn’s disease can present with cramping and irregular bowel habits, particularly in earlier stages, that mirror an IBS pattern closely. The NIDDK notes that a thorough IBS evaluation looks at health history and patterns that may point toward inflammatory bowel disease or other digestive conditions.
A symptom list alone rarely gives a complete answer. Within the digestive and metabolic health framework at Total Health Center, IBS evaluations look at what else may be contributing to the picture, because IBS and other digestive conditions can coexist, and identifying both produces a more complete path forward.
Get Personalized Digestive Support in Virginia Beach
When something in the symptom pattern feels different from the usual IBS experience, that observation is worth bringing to a clinician. Total Health Center offers a focused first visit built around health history and the specific pattern each patient presents. Call (757) 363-8571 to schedule.
Frequently asked questions
How do I know when my symptoms go beyond IBS?
The clearest signals are changes in stool appearance, unexplained weight loss, nighttime diarrhea and persistent pain after a bowel movement. Any of these warrants a clinical evaluation.
Can IBS and another digestive condition exist at the same time?
Yes. Celiac disease and inflammatory bowel disease can coexist with IBS, which is one reason a thorough evaluation looks at the full picture.
Is it normal for IBS symptoms to change over time?
Intensity shifts with stress, diet and life circumstances. A meaningful change in the pattern itself, with new symptoms appearing or familiar ones behaving differently, is worth taking to a clinician.
