Contact Us
Tel: (757) 363-8571
Autoimmune conditions affect each person differently and often require ongoing management. Many individuals continue to experience fluctuating symptoms despite appropriate medical care. This often shows up as periods where symptoms feel manageable, followed by flares that are hard to predict or control.
Functional medicine offers a supportive framework that looks at factors influencing symptom patterns over time. The goal is not to replace medical treatment but to provide additional support by addressing how different body systems interact and what may be contributing to symptom variability.
Autoimmune Symptoms Reflect More Than Immune Activity Alone
Immune activity is influenced by multiple internal systems. Inflammation, digestion, stress response, and metabolic balance can all affect how symptoms present and how intensely they appear.
This helps explain why symptoms may change even when treatment remains consistent. A flare isn’t always caused by disease progression. It can reflect temporary shifts in stress levels, sleep quality, digestive function, or other factors that influence immune regulation.
Understanding these connections doesn’t change the diagnosis, but it can provide insight into what may be amplifying symptoms at any given time.
Signs That Other Factors May Be Affecting Your Symptoms
In clinical practice, certain patterns suggest that factors beyond immune activity are influencing symptom severity. These aren’t diagnostic criteria, but they can indicate where additional evaluation may be helpful.
Patterns often seen in autoimmune cases:
- Flares that coincide with digestive symptoms (bloating, irregular bowel habits, food sensitivities)
- Symptom worsening during periods of high stress or poor sleep
- Fatigue that feels disproportionate to disease activity
- Difficulty recovering from minor illnesses or physical exertion
- Symptoms that improve temporarily with dietary changes but return without clear cause
These patterns don’t mean the autoimmune condition isn’t real or properly treated. They suggest that other systems may be under strain and affecting how the immune system behaves.
What We Evaluate for Autoimmune Support
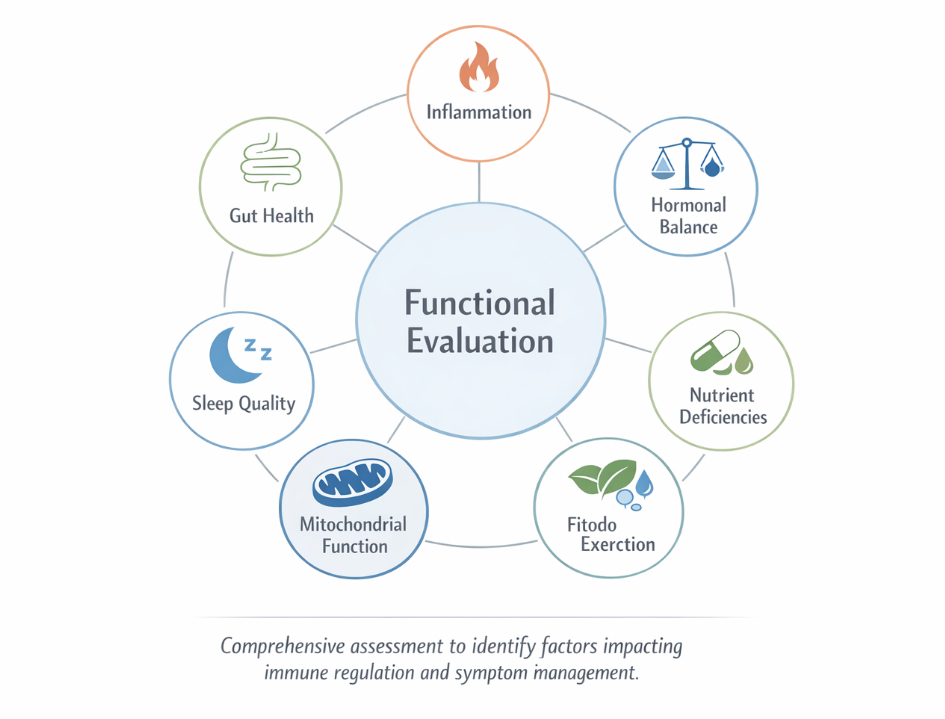
A functional medicine evaluation for autoimmune support looks at areas that standard care may not address in depth. The goal is to identify what might be maintaining inflammatory response or triggering immune reactivity beyond the autoimmune process itself.
Common areas of focus include:
- Gut barrier function: Intestinal permeability can influence immune activation. When the gut lining is compromised, larger molecules may cross into the bloodstream and trigger immune responses.
- Inflammatory triggers: Food sensitivities, environmental exposures, chronic infections, and toxin burden can all contribute to chronic inflammatory signaling that amplifies autoimmune activity.
- Hormonal regulation: Thyroid function, cortisol patterns, and sex hormones influence immune regulation. Imbalances in these areas often worsen autoimmune symptoms.
- Nutrient deficiencies: Vitamin D, omega-3 fatty acids, B vitamins, magnesium, and other nutrients play roles in immune modulation. Deficiencies can make symptoms harder to control.
- Mitochondrial function: Energy production at the cellular level affects how well the body manages inflammation and repairs tissue damage.
- Sleep quality and recovery: Poor sleep can increase inflammatory activity and weaken immune regulation, making symptoms harder to manage.
Testing is selective and based on clinical presentation. Not everyone needs every test. The evaluation is guided by symptom patterns, health history, and what’s most likely to provide useful information for that individual.
Tracking Patterns Can Help Identify Contributing Factors
When managing autoimmune conditions, understanding how lifestyle factors interact with symptoms can make a significant difference in treatment outcomes. Key elements such as nutrition, stress, sleep quality, and digestive health often contribute to the fluctuations in symptoms that patients experience. By monitoring these patterns over time, patients can begin to identify what may be triggering or worsening their condition, enabling a more personalized approach to care.
This process of identifying contributing factors goes beyond simply managing symptoms. It provides valuable insights into how various body systems interact, helping both patients and practitioners pinpoint areas that may need additional support. These insights can then inform treatment strategies that complement traditional medical care, promoting better overall health and symptom management.
Living With Autoimmune Conditions Requires Ongoing Balance
Autoimmune conditions are rarely static. Management often involves adjustment over time as the body changes, as life circumstances shift, and as different factors come into play.
A broader, whole-person perspective can be especially relevant in long-standing or complex cases. When standard treatment provides some benefit but symptoms still interfere with daily life, additional supportive care may help reduce that interference.
Functional medicine doesn’t promise resolution. It provides a framework for understanding what may be maintaining instability and what can be done to support better regulation over time.
How Supportive Care Fits Into Autoimmune Management at Total Health Center
Total Health Center has worked with individuals managing autoimmune conditions for over 28 years, often in cases where symptoms remain challenging despite ongoing medical care. The focus is on whole-person health and long-term management within a functional medicine framework.
Supportive care is provided alongside conventional medical care. The approach considers how inflammation, metabolic balance, stress response, and digestive function may be influencing symptom patterns. Testing may be used selectively to clarify what standard evaluations have not addressed.
Care is adapted over time based on how the body responds. Some individuals see improved stability relatively quickly; others require longer-term support as multiple systems are gradually brought into better balance. The emphasis is on sustainable improvement and realistic expectations.
Schedule a Functional Medicine Evaluation for Autoimmune Support
Total Health Center offers functional medicine care for individuals seeking a supportive, whole-person approach to autoimmune conditions. The initial visit includes a comprehensive health history, discussion of symptom patterns, and evaluation of factors that may be contributing to instability.
Appointments can be scheduled by calling the office or booking online. Care is designed to work alongside existing medical treatment, with attention to long-term stability and overall health.
