Vitamin D: One of the Most Overlooked Foundations of Health
Vitamin D deficiency is incredibly common—far more common than most people (and even many clinicians) realize. In my practice, I routinely see patients with low or suboptimal vitamin D levels, even those who “eat well” and consider themselves healthy.
Despite the name, vitamin D is not really a vitamin at all. It functions more like a steroid hormone, influencing gene expression throughout the body. In fact, vitamin D receptors are found in nearly every tissue, which helps explain why deficiency is linked to such a wide range of health problems.
When vitamin D levels are optimized, we see benefits far beyond bone health—supporting immune function, cardiovascular health, metabolic balance, and even cancer prevention.
Why Vitamin D Matters So Much
Vitamin D plays a role in regulating hundreds of genes involved in:
-
Immune defense against bacteria and viruses
-
Inflammation control
-
Cell growth and repair
-
Calcium balance and bone strength
-
Muscle function
-
Cardiovascular health
Low vitamin D levels have been associated with increased risk of infections, autoimmune disease, cardiovascular disease, mood disorders, chronic pain, and several types of cancer.
Vitamin D Deficiency Is Widespread
Large population studies have shown that vitamin D deficiency is the norm—not the exception:
-
Roughly one-third of U.S. adults and children are deficient
-
Up to 70% of school-aged children are deficient or insufficient
-
About half of the general population is considered at risk
One important point I emphasize with patients:
“Normal” does not necessarily mean “optimal.”
Many lab reference ranges are based on average values from a population that is already deficient.
What Is an Optimal Vitamin D Level? 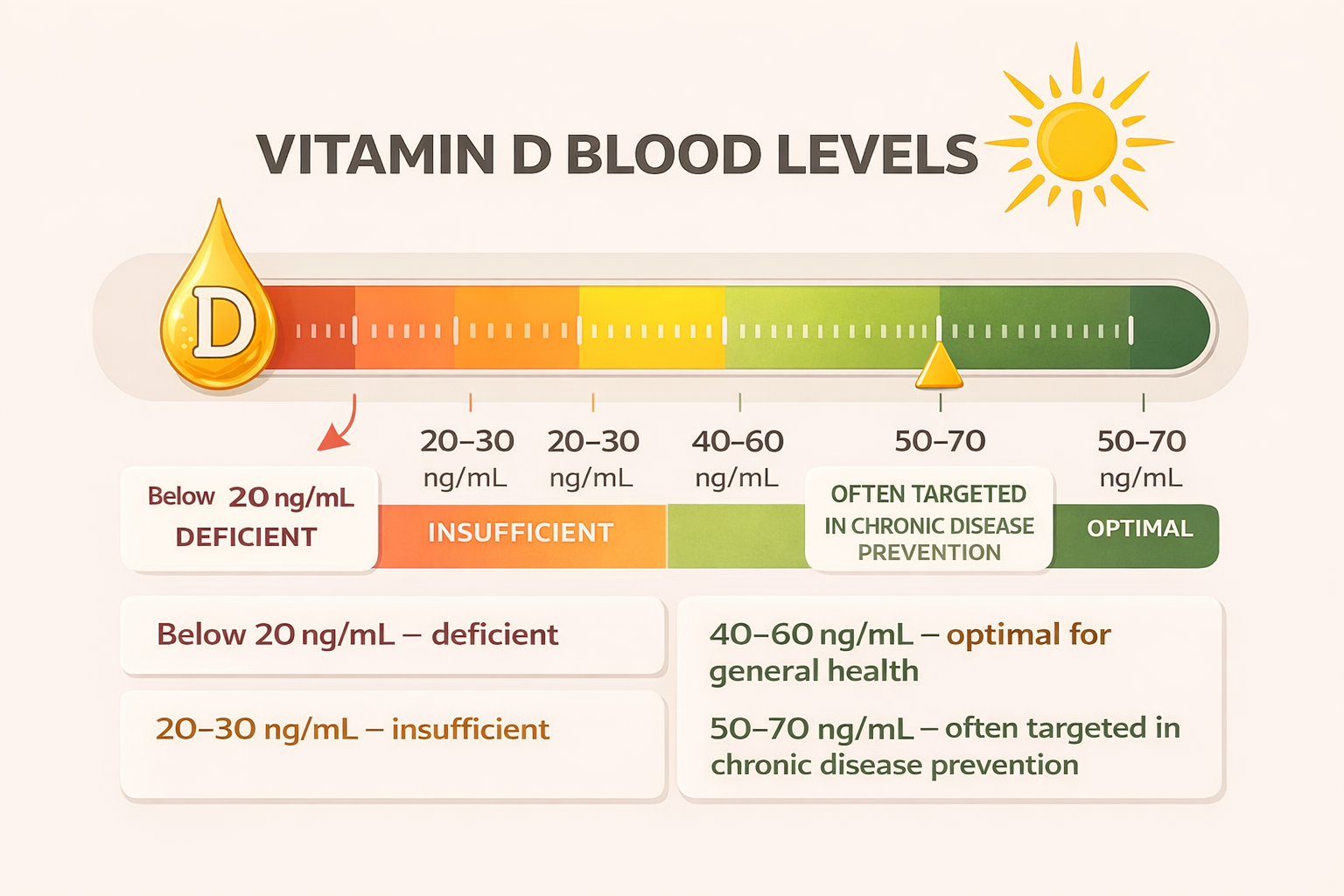
Vitamin D status is measured by a blood test called 25-hydroxyvitamin D.
Based on populations with regular sun exposure and current research, most experts agree:
-
Below 20 ng/mL – deficient
-
20–30 ng/mL – insufficient
-
40–60 ng/mL – optimal for general health
-
50–70 ng/mL – often targeted in chronic disease prevention
This is why testing matters. The “right” dose of vitamin D varies widely from person to person.
Sunlight: The Most Natural Source of Vitamin D 
Whenever possible, sun exposure is the best way to optimize vitamin D.
When your skin is exposed to UVB rays, your body produces vitamin D in a form that lasts longer in the bloodstream than supplements. Sun exposure also triggers other beneficial compounds in the skin that we don’t get from pills.
General guidelines for sensible sun exposure:
-
Expose arms, legs, abdomen, and back
-
2–3 times per week
-
About half the time it would take to burn
-
Best window: late morning to early afternoon
Important notes:
-
You cannot make vitamin D through glass
-
Early morning and late afternoon sun produces little to no vitamin D
-
During daylight saving time, peak sun exposure is closer to 1:00 pm, not noon
If you live in northern latitudes, meaningful vitamin D production from sunlight is usually not possible from late fall through early spring.
What About Tanning Beds?
If sunlight is truly unavailable, certain tanning beds that emit UVB (not just UVA) can increase vitamin D levels. However, not all tanning beds are created equal, and this approach should be used cautiously and selectively.
Protecting the face and limiting exposure time is critical.
Vitamin D Supplements: When Sun Isn’t Enough
If adequate sun exposure isn’t realistic, vitamin D3 supplementation can be very helpful.
General dosing ranges often used:
-
Children: 600–1,000 IU daily
-
Adults: 1,500–2,000 IU daily (minimum)
-
Many adults require 3,000–4,000 IU daily to reach optimal levels
People with obesity, chronic illness, or malabsorption often need higher doses.
A commonly used estimate is ~35 IU per pound of body weight, but testing is still the best guide.
Vitamin D can be taken daily, weekly, or monthly, but I generally prefer daily dosing for consistency.
Don’t Forget Vitamin K2
If you supplement with vitamin D—especially at higher doses—vitamin K2 is essential.
Vitamin D increases calcium absorption. Vitamin K2 ensures that calcium goes into bones and teeth, not into arteries or soft tissues.
Without adequate K2, calcium can end up in the wrong places, which is why vitamin K2 deficiency—not vitamin D itself—is often behind concerns about calcification.
Think of them as a team:
-
Vitamin D increases calcium availability
-
Vitamin K2 directs calcium where it belongs
Fatigue, Aches, and Chronic Pain? Check Vitamin D
Low vitamin D can cause deep, aching bone pain, muscle weakness, and fatigue—symptoms often mislabeled as fibromyalgia or chronic fatigue.
Correcting vitamin D deficiency (along with adequate magnesium and dietary calcium) can be life-changing for some patients.
Vitamin D Across the Lifespan
Vitamin D is critical from pregnancy through old age.
Research links deficiency to:
-
Pregnancy complications such as pre-eclampsia
-
Increased risk of C-section
-
Childhood asthma and autoimmune disease
-
Higher lifetime risk of diabetes, MS, and inflammatory bowel disease
Optimizing vitamin D status early may have profound long-term health effects.
The Bottom Line
Vitamin D is one of the simplest, most affordable, and most powerful tools we have for supporting long-term health.
Whether through smart sun exposure, supplementation, or a combination of both, maintaining optimal vitamin D levels should be a foundational part of any preventive or functional medicine approach.
If you haven’t checked your vitamin D level recently—or ever—it’s worth discussing with your healthcare provider.
Sometimes, small changes truly make a big difference.
CLICK ON THE IMMAGE TO GO TO THE STORE.
Or call the office to order. (757)363-8571