When most people are diagnosed with Type 2 diabetes, the conversation quickly turns to one thing:
👉 Insulin
But here’s the truth…
Insulin is often used to manage blood sugar—but it does not address the underlying cause of Type 2 diabetes.
And in many cases, there’s a deeper issue driving the condition:
👉 Chronic inflammation and metabolic dysfunction
Insulin: Management Tool vs Root Cause Solution
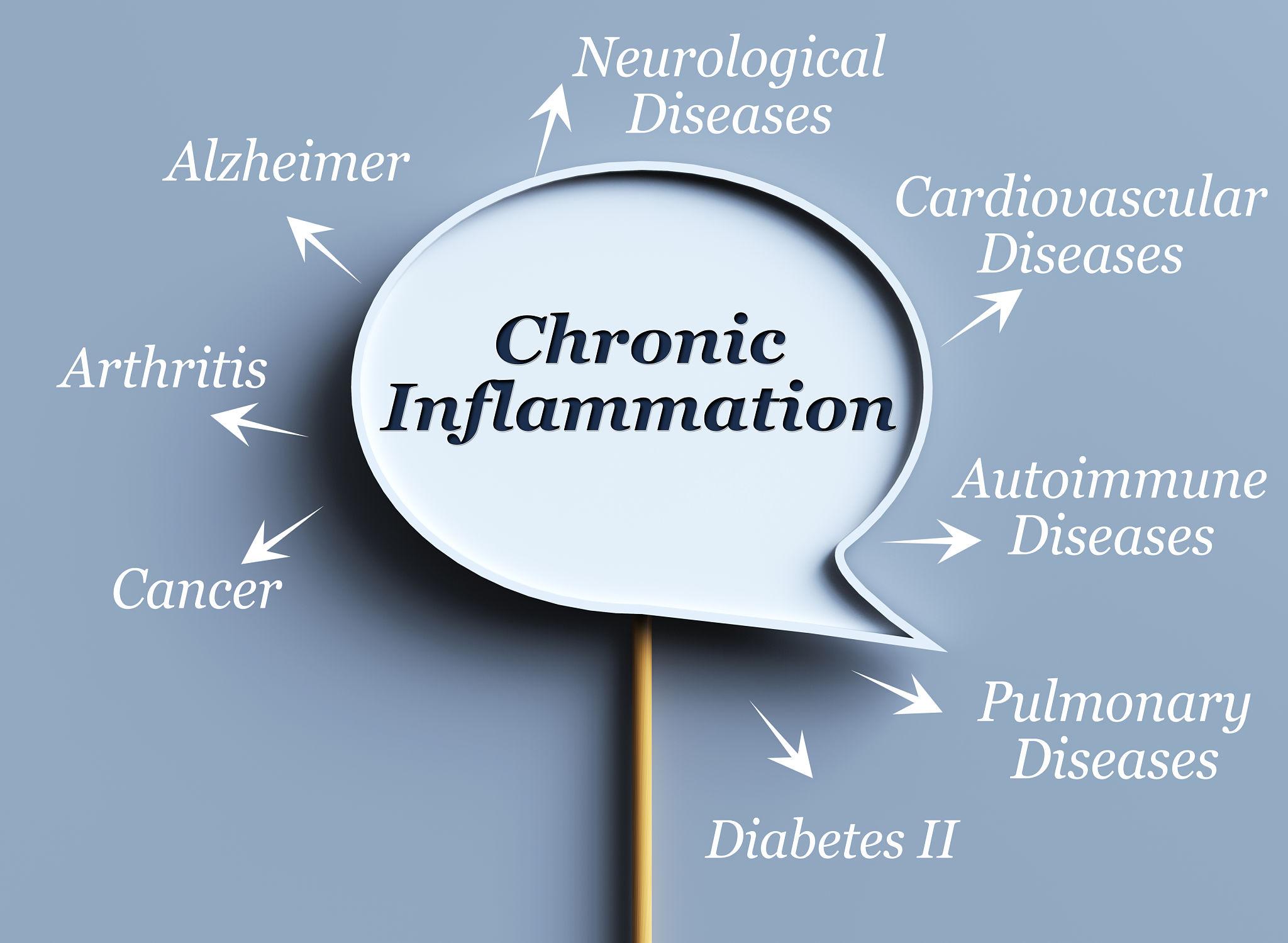
Chronic inflammation plays a major role in insulin resistance and metabolic dysfunction
Insulin plays an essential role in the body:
- It helps move glucose into cells for energy
- It regulates blood sugar levels
And in some cases, it is absolutely necessary.
But in Type 2 diabetes, the real problem is often:
👉 Insulin resistance
This means:
- The body is already producing insulin
- But the cells are not responding properly
Adding more insulin may lower blood sugar…
…but it doesn’t fix the underlying dysfunction.
The Hidden Link: Inflammation and Diabetes
Chronic inflammation is a major driver of:
- Insulin resistance
- Weight gain
- Cardiovascular disease
Research shows that elevated inflammatory markers are associated with worsening metabolic health.
Some key contributors to inflammation include:
- High sugar intake
- Processed foods
- Chronic stress
- Poor sleep
The Role of Cortisol (Stress Hormone)
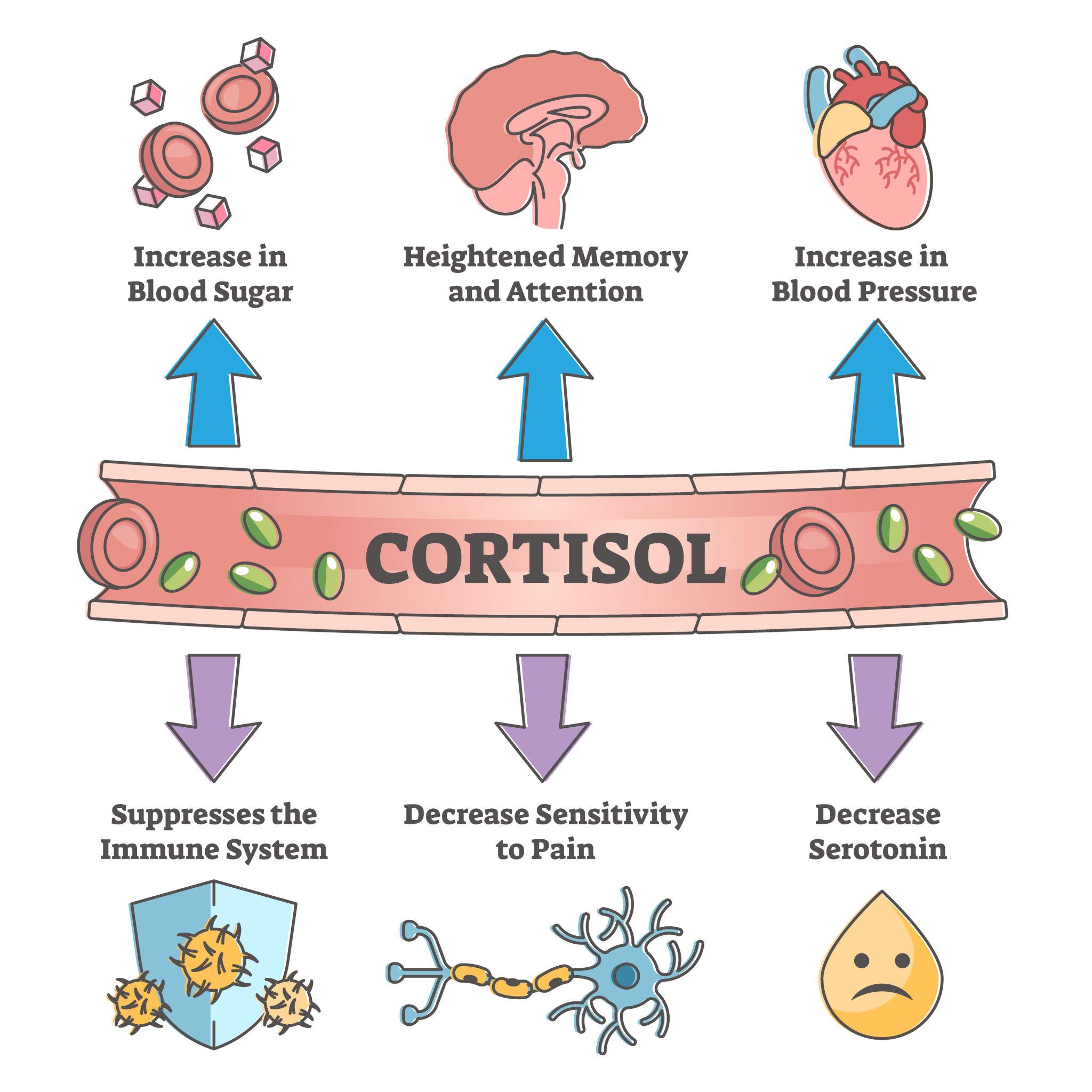
Chronic stress and elevated cortisol can worsen blood sugar control
Cortisol, produced by the adrenal glands, has a direct impact on blood sugar.
When cortisol is elevated:
- Blood sugar increases
- Insulin resistance worsens
- Fat storage increases
This is why stress management is a critical—but often overlooked—part of diabetes care.
Diet and Inflammation

The Standard American Diet (high in refined carbohydrates and processed foods) fuels inflammation.
A better approach includes:
- Vegetables
- Lean proteins
- Healthy fats
- Nuts and seeds
What about fruit?
Fruits can be part of a healthy diet—but for diabetics:
- Focus on lower glycemic options
- Pair with protein or fat
- Monitor blood sugar response
Key Lab Markers for Inflammation
Advanced lab testing helps uncover hidden inflammation and metabolic dysfunction
To truly understand what’s happening, we look beyond glucose.
Important markers include:
C-Reactive Protein (CRP)
A general marker of inflammation in the body.
Homocysteine
Elevated levels are associated with:
- Cardiovascular risk
- Cognitive decline
Many functional medicine practitioners aim for:
- Optimal levels below ~7
Ferritin
Ferritin reflects iron storage, but:
- It can also rise with inflammation
- Interpretation must be done carefully
The Bigger Picture
Type 2 diabetes is not just a blood sugar problem.
It’s a metabolic and inflammatory condition.
Focusing only on glucose levels without addressing:
- Diet
- Stress
- Inflammation
- Lifestyle
…means you’re missing the root cause.
A Functional Medicine Approach
At Total Health Center Virginia Beach, we take a deeper approach.
We focus on:
- Identifying underlying causes
- Reducing inflammation
- Restoring metabolic balance
Not just managing numbers—but improving overall health.
If you’ve been told your diabetes is “under control” but you still struggle with:
- Fatigue
- Weight gain
- Brain fog
- Cravings
There’s more to the story.
👉 Call 757-363-8571 to schedule your FREE consultation
Let’s uncover the root cause and build a plan that actually works.

